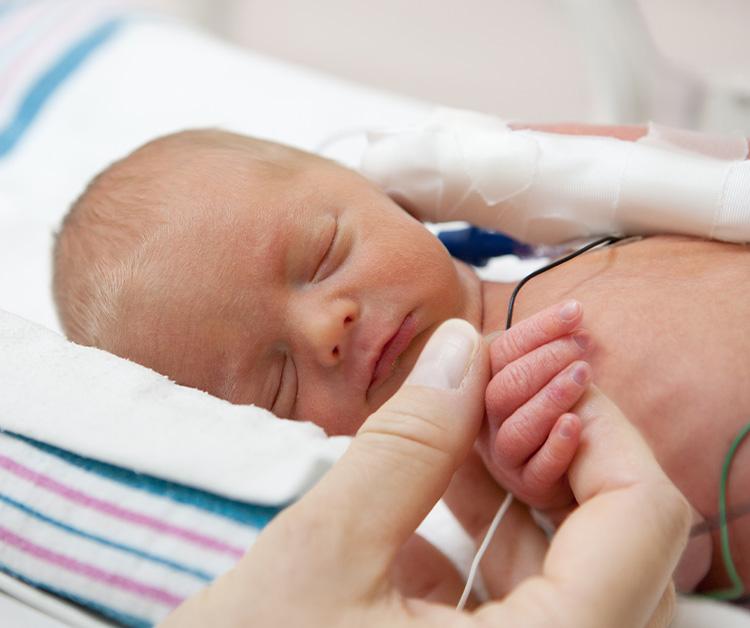
New methods to treat the potential medical problems faced by premature babies are constantly evolving. Here's an introduction to a few areas that the NICU staff will be monitoring for your baby.
Neonatology is a rapidly changing field of medicine, and there are bound to be variations from hospital to hospital in terminology, technology, and treatments. Your doctor may use slightly different terms to describe some of the medical conditions discussed here. However, this basic information may help you begin to build your understanding of caring for premature babies.
A premature baby, especially a baby with breathing problems, is marginally supplied with calories and oxygen—the fuels they need to heat their body. A main objective of your NICU staff is to keep your baby warm—but not too warm. Your baby will mostly likely be placed in an incubator or warmer, so that their temperature may be carefully controlled.
A tiny device that acts as a thermometer may be taped over your baby's belly. It constantly senses your baby's temperature and regulates the temperature of the environment within the incubator. It will increase the warmth when your baby gets too cool and decrease it when they're too warm.
Your baby's axillary (under the arm) temperature will be checked frequently, as well. For more added warmth, and also to keep them from grabbing or kicking tubes and wires, your baby may also be dressed in mittens, booties, and a hat.
The goal is to keep your baby's body temperature as close to normal as possible—98.6°F (37.0°C). This is also the temperature at which they conserve the most oxygen and calories and gain the most weight.
It's very common for a premature baby to have breathing problems. The severity of the problem may depend on how prematurely your baby was born. A premature baby's lungs aren't as fully developed and ready to breathe as a full-term baby's. Let's look now at some common problems associated with breathing.
Apnea is the term used to describe the times a baby interrupts breathing. Apnea is a very common problem faced by premature babies in the early weeks of life. Apnea is often accompanied by bradycardia—a lower-than-normal heart rate. For a tiny baby this means the heart is beating fewer than 100 times a minute. This is considered slow for a baby, even though an adult heart rate is usually much slower.
RDS is a breathing disorder found in premature babies. It is caused by the baby's inability to produce surfactant—the fatty substance that coats the alveoli (the tiny air sacs in the lungs) and keeps them from collapsing. An unborn baby's lung tissue begins making small amounts of surfactant in the early weeks of pregnancy, but most babies aren't producing enough surfactant for proper breathing until the 35th week of gestation. However, since babies do vary greatly in their rates of lung development, some premature babies have enough surfactant to breathe without difficulty while others do not. In general, the more premature the baby, the greater the risk of developing RDS.
If it is necessary for your baby to be on a respirator (breathing machine), the pressure may occasionally cause air to leak from their lungs. Tiny air bubbles may be forced out of the alveoli and in between layers of lung tissue. This condition, called pulmonary interstitial emphysema (PIE), usually subsides as your baby's respiratory problems improve and respirator pressure to the lungs can be reduced. Sometimes a tear can occur and leak into the surrounding chest spaces causing the lung to collapse. This is the condition called pneumothorax.
More than half of all full-term babies and more than three-fourths of all premature babies get
during the first three to seven days of life. This isn't a reason for concern most of the time, although it does cause the baby's skin and whites of their eyes to turn somewhat yellow.Babies are born with a large number of fetal red blood cells. Normally, as red blood cells break down, bilirubin, which is a yellowish pigment, forms. The bilirubin is detoxified (processed) in the liver. If the enzymes in the liver that process the bilirubin aren't working efficiently yet (which happens often in newborns and especially in premature babies) the bilirubin level rises in the blood and some of it enters body tissue, where it then temporarily causes a yellowing—the condition called jaundice.
While in the NICU, your baby's blood will be frequently checked for a rise in bilirubin. If the levels rise closer to those that are considered unsafe, they may be treated by phototherapy (most common) or transfusion.
If your baby is in the NICU, chances are they will need to receive some type of medication, nutrients or perhaps blood. There are two common ways medicine is provided to your baby in the NICU.
The umbilical arterial catheter is inserted through the end of a baby's umbilical cord (at the belly button) and is threaded through the umbilical artery into the aorta, the main artery supplying the body with oxygenated blood. While this sounds painful, it really isn't. There are no nerve endings in your baby's umbilical cord where the catheter (tiny tube) is inserted.
An IV pump is a machine attached to a pole placed near your baby's bed. IV stands for intravenous (in´-trah-vee´-nous), which means into the veins.
These are just some examples of common problems faced by premature babies. Learn more ways you can help care for your newborn and be sure to talk to your baby's doctor about their approach to caring for premature babies in the NICU and beyond.
All information on Enfamil, including but not limited to information about health, medical conditions, and nutrition, is intended for your general knowledge and is not a substitute for a healthcare professional's medical identification, advice, or management for specific medical conditions. You should seek medical care and consult your doctor or pediatrician for any specific health or nutrition issues. Never disregard professional medical advice or delay seeking medical treatment, care, or help because of information you have read on Enfamil.